Welcome to The Thyroid guide! I am super happy to have you here and I really hope you find this guide helpful! If you need to reach out to me you can email me at support@chemainesmodelhealth.com , you can find me on Facebook and here in our Facebook group – https://www.facebook.com/groups/thethyroidguide/edit/ , where you will find extra information and support.
Most of us know about the Thyroid, know someone with Thyroid issues and may even believe we have Thyroid issues ourselves. And most people with low Thyroid symptoms aren’t detected until it’s too late and when they are detected, their only option is Synthroid.
Over 30 million people have undiagnosed Thyroid conditions…that’s crazy right?!
There are many natural strategies that address the root cause of your Thyroid issue and these can give your Thyroid the best chance to heal. That’s not to say that in some cases pharmaceutical intervention is not needed….but for many, a holistic functional approach can be enough to see improvements in both your Thyroid and health. In this guide we hope to teach you strategies that will have you feeling better than you have in years. Enjoy!
Module 1;
What is the Thyroid?
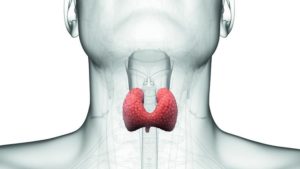
Your thyroid gland is a small gland shaped like a butterfly or bow tie, normally weighing less than one ounce, located in the front of the neck. It is made up of two halves, called lobes, that lie along the windpipe (trachea) and are joined together by a narrow band of thyroid tissue, known as the isthmus.
The thyroid is situated just below your “Adams apple” or larynx. During development (inside the womb) the thyroid gland originates in the back of the tongue, but it normally migrates to the front of the neck before birth. Sometimes it fails to migrate properly and is located high in the neck or even in the back of the tongue (lingual thyroid). This is very rare. At other times it may migrate too far and ends up in the chest (this is also rare) but still good to know 🙂 .
One of the key functions of the thyroid is to drive your metabolism. If your metabolism is slow, fat burning becomes difficult. Sure, you hit the gym, run the kilometers and watch your diet — but if your thyroid is low/slow, you will only be burning fat optimally during these periods of exercise. Even if you exercise for one hour a day, that is still less than 5% of your day you are burning fat effectively. If you had an optimal metabolism and thyroid function, you would be burning fat for 24 hours a day, 7 days per week plus having more energy. How awesome would that be?
But what causes your Thyroid to slow down or not function properly? Well there are many thing and the biggest players in my opinion are stress and toxic exposure….but other causes include;
- weight gain or obesity
- trauma
- genetics
- adrenal issues
- nutrient deficiencies, especially iodine
- excessive fluoride exposure
- estrogen dominance
- chronic inflammation
- insulin resistance
- breast implants
- illness
- poor gut health including IBS and Celiac disease
- poor liver health
- lack of sleep or chronic fatigue
- *iodine deficiency is one of the leading causes of hypothyroidism in many underdeveloped countries and can also lead to goiters.
Symptom picture checklist for slow or under-active thyroid function
- generalized weight gain that is difficult to account for and lose
- fluid retention
- fatigue
- trouble falling asleep and staying asleep
- apathy and depression
- too tired and cranky to care or tolerate ‘idiots’ (impatient towards others)
- cold or overly sensitive to cold breeze, drinks and foods
- cold hands and feet
- swollen and bloated regularly
- slow bowels with excessive bloating and gas and fullness
- constipation
- gallbladder or bile issues
- weakened immune
- poor circulation and fluid retention
- dry, weak and poor quality hair
- excessive hair loss
- loss of the tail end of your eyebrows
- dry skin
- red bumpy rash around the neck and inner arms
- weak, brittle or poor quality finger and toe nails
- sluggish bowels and constipation
- burping, farting and gurgling guts
- menstrual cycle irregularities
- fertility issues or trouble conceiving
Overview of Thyroid Hormone Production
So let’s outline how the thyroid hormonal cascade or domino really works. The first step we have is the brain signalling down to the thyroid. This pathway is known as our TSH or our thyroid stimulating hormone. Our TSH is coming from the brain particularly the pituitary and it’s telling the thyroid to make thyroid hormone.
Now from there, our thyroid then spits out some T4. About 20% of that T4 actually gets converted to T3 at the thyroid and we’ll review some of the nutrients that we need to help that conversion later in this guide. So 20% happens in the thyroid gland, then the other 80% happens peripherally (at tissue locations). So we look down at that 80%; 60% of that 80 happens at the liver, this is why it’s very important to always be supporting your liver. Then if we look at T2, this happens in the cells or mitochondria…more on that below.
The Thyroid hormones;
T4 (Thyroxine)
T4 is virtually the building blocks to the ‘active’ thyroid hormones. T4 has only 1/10th the activity of T3. A form of T4 is the synthetic drug (Oroxine) commonly prescribed by medical doctors for people with low thyroids. When an iodine is removed from T4 and converted to T3, the hormone becomes vastly more active.
T3 (Triiodothyronine)
T3 is the major pace maker of the body binding to nuclear receptors (thyroid hormone receptors). It regulates resting metabolic rate (increases the minimal level of calories that a person needs in order to sustain life while resting), thermogenesis, heart rate, increasing the consumption of both oxygen and energy in the body, the synthesis and degradation of the macromolecules, increase the rate of protein degradation and synthesis and controls the growth of bones.
rT3 (Reverse T3)
T4 can convert down two different pathways; either conversion to T3 or Reverse T3. T3 is 7x more potent thermogenic than T4. Reverse T3 is 1/100th as potent as T4 as a thermogenic and will bind and block the T3 receptors preventing the thermogenic T3 from acting directly and converting to the most potent thermogenic T2.
T2 (Diiodothyronine)
Until recent years, T2, because of its very low affinity for thyroid hormone receptors, was considered an inactive metabolite of thyroid hormones T4 and T3. Several observations, however, led to a reconsideration of this idea. T2 rapidly stimulates cellular mitochondrial respiration regulating thermogenesis/metabolism and energy expenditure…..whoop for fat burning. T2 also has the ability to reduce adiposity and dyslipidaemia (fat in the blood) and to prevent the development of liver steatosis (fatty liver) showing a rapid T2-induced increase in the ability of mitochondria to import and oxidize fatty acids (use fat for energy).
Thyroid hormones for fat loss
Thyroid hormones control your metabolic rate, digestive function and thermogenic activity. It is essential to control the thyroid hormone pathways to ensure that it works optimally as a potent thermogenic compound. There are many factors that will alter the thyroid hormone conversion pathways as we saw above (and we will look at more throughout this guide). But ere is your basic strategy to support your thyroid function.
- Support healthy thyroid hormone profile
- Maximize Thyroxine (T4) production and release
- Enhance the conversion of T4 to the more active form Triiodothyronine (T3)
- Boost the thermogenic form or production of thyroid hormone, Diiodothyronine (T2)
- Reduce reverse T3 (rT3) (a potential suppressor of thyroid function)
Thyroid Testing
Thyroid autoimmunity or Thyroid dysfunction is a big issue–40% of people that test for thyroid autoimmunity actually test a ‘false negative’. They may come back negative but they may still have a positive thyroid issue based on the symptom picture (symptoms listed above).
Lab tests are of little use when not combined with a symptom picture.
So make sure you get your thyroid looked at either palpation-wise and/or if you need, get an ultrasound run just to make sure there are no nodules or inflammation in the thyroid that could be caused by Hashimoto’s and a full blood or hormone panel done, that includes the below tests, which MUST be combined with your symptom picture; *number ranges are holistic or functional medicine based.
- TSH or Thyroid Stimulating Hormone – 0.5-1.5 mlU/L
- Free T4 or Free Thyroxine – 1.3-2.8 ng/dL
- Free T3 or Free Triiodothyronine – 3.7-4.2 pg/mL
- Reverse T3 (this is an inactive hormone that slows the Thyroid) – FT3 to RT3 ratio should be greater or equal to 20
- TPO or Thyroid Peroxidase – <2 IU/mL
- TG or Thyroglobulin – <2 IU/mL
Some doctors will do this full panel willy nilly but others may decline or ask you to pay for them. Regardless, you should push for them to get done and then have them reviewed and compared to your symptom picture. That way you can get an accurate diagnosis and start to put together a plan of action that will address your individuality.
What is the difference between Hypothyroidism and Hashimotos?
This is really just a side note or little extra knowledge but its good to understand the differences.
Hypothyroidism, by definition, is a clinical state. It is a state of a slow functioning thyroid or low levels of thyroid hormone in the body.
The low levels of thyroid hormone can occur as a result of a variety of different reasons, such as iodine and other nutritional deficiency, surgical removal of the thyroid, excess use of thyroid suppressing medications, pituitary suppression (from stress or malnutrition), Hashimotos or damage to the thyroid (physical or disease induced).
Hashimotos thyroiditis is an autoimmune condition, that results in the destruction of the thyroid gland. This damage eventually leads to inadequate thyroid hormone production, or hypothyroidism. Hashimotos usually begins as a gradual enlargement of the thyroid gland, which is sometimes detectable by the individual on self examination. It can be accompanied by hoarseness and or breathing difficulty’s. When damage to the gland is just beginning, the body compensates and produces more hormone, thus keeping the hormone levels in “normal” range. But the person may start or be experiencing symptoms of hypothyroidism…..This is mild hypothyroidism, whereas others might experience too much thyroid hormone or thyrotoxicosis. This beginning stage is diagnosed as “subclinical” hypothyroidism — defined as increased TSH levels accompanied by “normal” T4 and T3. *Hashimotos is the most common cause of hypothyroidism is the United states, accounting for about 90%.
A good doctor will test you for Hashimotos too if they feel there might be a hypothyroidism diagnosis.
You doctor can test for thyroid antibodies, and when they identify their presence, they can put corrective actions in place, so thyroid disease doesn’t manifest or progress. Thyroid antibodies are going to be the first indication of a thyroid problem in many cases. They can be elevated for 5, 10, sometimes even 15 years before a change in TSH is even detected!
There are three main types of antibodies in Hashimoto’s that are potentially going to be present. Two of them are created by the immune system to target the thyroid gland as if it were a foreign invader like a pathogen, and those are Thyroid Peroxidase (TPO) and Thyroglobulin (TG) antibodies.
80-90 percent of people with Hashimoto’s will have either TPO or TG antibodies, or both. The more elevated the thyroid antibodies are, the greater the likelihood of developing overt hypothyroidism as well as possibly additional autoimmune conditions.
The third type of thyroid antibodies is TSH-Receptor (TSH-R) antibodies, including thyroid-stimulating immunoglobulin (TSI). This particular marker is elevated in more than 90 percent of people with Graves’ disease. TSH-R antibodies are also more common in people who have thyroid cancer.
Triggers for Hashimotos can be food sensitivities, nutrient depletions, toxin exposures, chronic infections, a poor stress response, and a number of other things. Some triggers can actually also lead to intestinal permeability (leaky gut) issues as well, such as with what happens with gluten sensitivity. So gastric distress or gut issues can be a sign that something is going on.
OK I think we will leave that there, as that is a good amount of knowledge for you to move forward with for a diagnosis or to understand your diagnosis a bit more. When your ready, you can move onto week 2, where we will look at; how to start supporting your thyroid through nutrition (what to eliminate and what to add in) and supplementation. And what exercise should or shouldn’t you do for thyroid health.
Regards,